Solutions
an independent leader in third-party benefit administration
Delta Health Systems comes with a myriad of solutions for healthcare on your terms and our commitment to you is what sets us apart.
customer service
Delta Health Systems is here to serve as an extension of your existing staff. Our commitment to you includes outstanding customer service, which features:

A unique toll-free number for each client, with direct access to a team of customer service representatives and claims processors

Plan administration

Online plan performance, business solutions and experience reports
audits
We will provide your employees with prompt, accurate, and effective service. To maintain our high standards, we frequently conduct internal audits for claims processing, eligibility maintenance and phone etiquette. Our audits include:

In-House Auditor Reviews

EDI Claims Directly from Providers

Claims Scanning with Optical Character Recognition (OCR) for Data Entry

HIPAA Compliant Transactions
call services
Tracking Client Calls
Customer service inquiries and resolutions are tracked internally, including issues related to eligibility, benefits, and decision outcomes. The number of calls, hold/call times, and dropped calls are also recorded.
Customer Service Representatives
Our staff is trained to handle a variety of customer service calls, including claim status, eligibility, and benefit inquiries.
Our staff has:
- The authority to reprocess and make adjustments to claims, as appropriate.
Note: Significant requests are overseen by management. - This higher level of authority increases the first call resolution rate and level of customer satisfaction.
- The ability to view scanned images of provider claims, Explanation of Benefits (EOBs), scanned correspondence, and processed payments.
- The ability to view client plan provisions and important documents such as SPD, SBC, and amendments.
bilingual services
Bi-Lingual Customer Service Representatives
Delta recruits and trains Spanish-speaking service representatives to ensure our participants’ needs are understood and met. For clients that have a large number of Spanish-speaking employees, we have the ability to generate EOBs, COB, TPL, SPDs, COBRA, HIPAA, FSA, and welcome packets in Spanish and/or English.
Website Services for Members
At www.deltahealthsystems.com, our customers can verify eligibility, claim status, and view plan benefits. In addition, members can print HIPAA privacy and claim forms, order temporary ID cards, print EOBs, find a provider, and contact customer service. Enrolled members can also utilize online, interactive wellness and disease management tools.
E-Sign Documents on our Website
For your convenience, you can sign forms electronically through our partnership with EchoSign—no more waiting for documents, scanning, or faxing signature pages.
We have standard forms available for registered members, such as Coordination of Benefits (COBs), Third Party Liability, and Authorization of Designated Representative for e-signature utilizing EchoSign digital documents. Members must be signed into our website to use the digital signature service.
Delta Health Systems provides proven expertise to administer and manage consumer-directed health plans (CDHP), as well as comprehensive spending account administration for all categories of medical savings accounts:
- Flexible spending accounts (FSA).
- Health reimbursement accounts (HRA), and
- Health savings accounts (HSA)
These plan designs help turn passive members into active participants by helping them manage their health and the related costs.
Participants are empowered to take control of their healthcare spending, including:
- A debit card to use at the pharmacy, doctor’s office or hospital for payment.
- Customer service support and record keeping.
- Integrated PPO Plan administration with FSA, HRA, and HSA processing.
- Ability to stack consumer products (FSA/HRA/HSA), including fund sequence, roll over, allocation, and usage options.
- Medical bill review and payment with EOB production.
Healthy Rewards emphasizes and rewards impactful consumerism, and also raises health awareness. Chronic diseases are steering healthcare costs over the cliff. Healthcare costs for chronic disease treatment account for more than 75% of health expenditures; an expense shared by employers and employees. These common and costly diseases are often treatable, or completely preventable, when people pursue a healthy lifestyle.
Healthy Rewards incents members to participate by reducing their contribution levels—up to 30% of the benefit value.
The key components of the plan are:
- Programs that provide a clinical benchmark and annual results for each member
- Care management tools to assist with positive behavior change
To see how Healthy Rewards could work for you, contact sales at sales@delapro.com or call 866.724.0032.


Delta Health Systems offers a variety of options that promote wellbeing. Our TeamCare programs empower our members to achieve healthy outcomes, while preventing claims and reducing healthcare spending. While these programs are not required, they are highly recommended to achieve the best results.
Employers can choose the TeamCare programs that are right for their organization.
a few of delta’s teamcare programs are:
utilization review

A URAC-accredited program that involves our specialized team of doctors and nurses who produce favorable patient outcomes at the lowest possible cost.
case management

URAC-accredited case management services focus on educating and helping members make choices that contribute to a healthier lifestyle, thus reducing the incidence of complications and future medical costs.
maternity management

Provide education and support to expectant mothers in order to reduce instances of complications and subsequent high claims costs.
disease management

Targets chronic conditions, such as diabetes and asthma; evidence-based guidelines are used to impact health and measure improvements.
telemedicine

A telehealth solution that offers a low-cost, convenient alternative to primary, emergency and urgent care visits; help employers improve employee health and productivity through telephone or secure video.
biometric screening

Provides unparalleled diagnostic accuracy, easy-to-understand online reporting, real-time tracking and integrated physician, nutritionist and lifestyle management coaching consultations

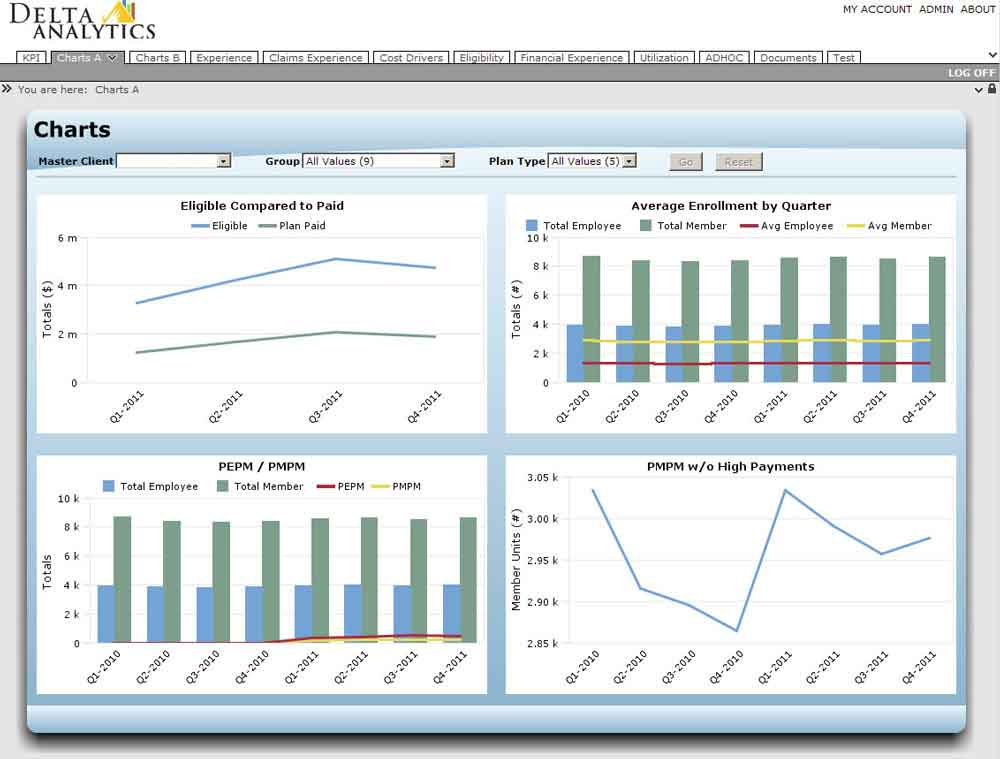
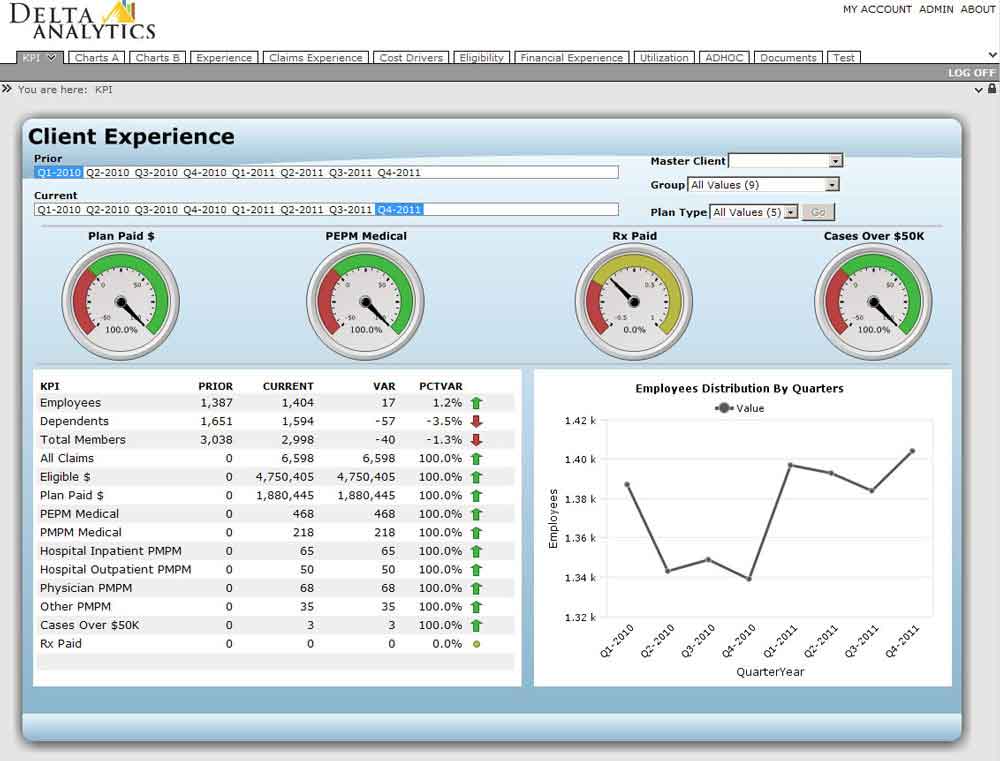
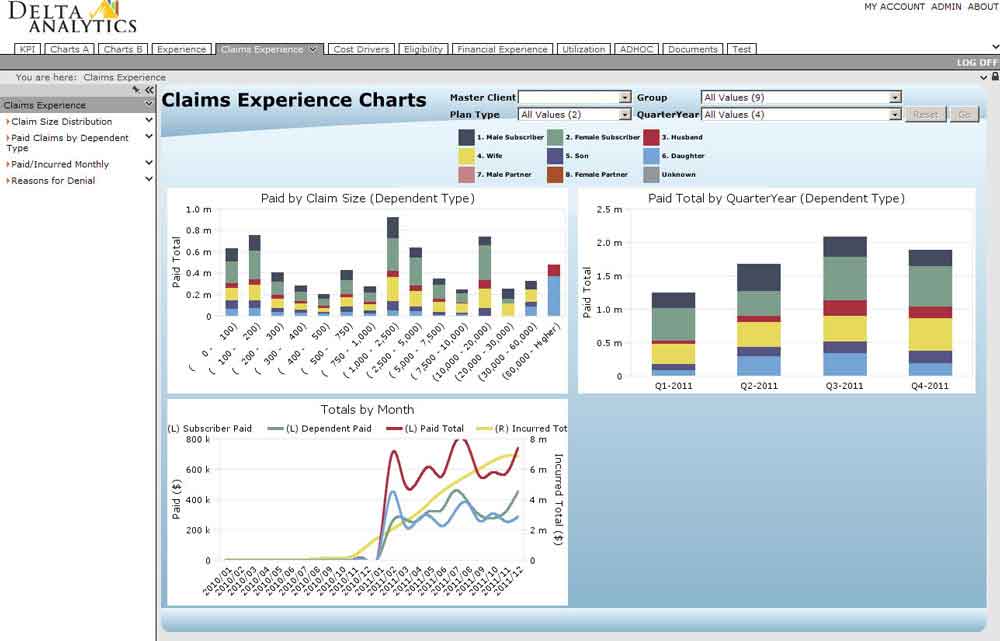
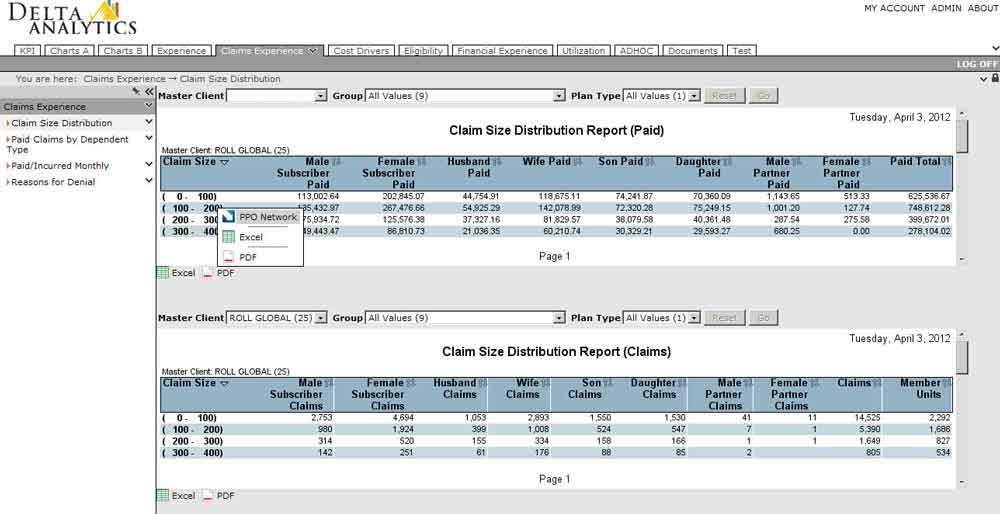
Delta Analytics is a robust reporting tool that provides you with a number of powerful analytical components that are highly customizable; data access control and encryption are all standard functionality. This end-to-end business solution delivers essential business intelligence to provide a return on your investment. Users have the ability to create their own ad hoc reports, utilize pre-defined reports, and analyze plan utilization and administration.
Our client service managers and executives are available to meet with your company on a quarterly basis, or as necessary, to provide reports and discuss plan performance. Our experience reporting provides insight into trends on utilization, as well as financial analysis and benchmarking. For groups of at least 1,000 employee lives, a more comprehensive report is completed prior to renewal.
purchase individual policies
Delta Health Systems understands the difficulty in finding cost effective health insurance for individuals and families. In the event you no longer have healthcare coverage through your employer, we have partnered with eHealthInsurance to provide a forum for seniors, individuals, and families to learn about, compare and apply for health insurance.
Offering the largest selection of health plans from leading insurance companies nationwide, the eHealthInsurance website features the following tools to assist you in finding the health plan that best meets your needs:

online instant quotes

side-by-side plan benefit and cost comparison

online physician directories

These features, along with online applications, make finding and purchasing the right health plan easier and more convenient than ever before. Visit www.eHealthInsurance.com today by selecting the product that meets your health insurance needs:
Note that there are many options for health insurance, and eHealthInsurance is one option for coverage. Qualified beneficiaries should review all of their options for health insurance, including special enrollment rights in other group health coverage, such as a spouse or parent’s plan. In addition, qualified beneficiaries can buy an individual health insurance policy through other insurance carriers and can check with their state’s Department of Insurance for assistance.
DISCLAIMER
Delta Health Systems and its employees are not liable for any direct, indirect, incidental, punitive or consequential damages of any kind whatsoever with respect to the service, materials or products obtained through any linked site.

Delta Fund Administrators (DFA) is the multiemployer and governmental plan account management company of Delta Health Systems. Formed in 2011, DFA is responsible for the strategic management and overall direction of the operations, contract administration, and financial management of each Plan/Fund ensuring consistency with the overall mission, goals and strategic objectives of the various Boards.
Delta Fund Administrators understands the unique needs and significant time required to provide account management to a multiemployer or governmental plan. The DFA service model combines people and systems. By assigning a team of people experienced in Trusteed plan administration focusing on the unique needs of these plans, Delta is creating the personal touch required in these relationships. Our account management expertise is then paired with the power of Delta Health System’s technology to bring you and your client unparalleled service and plan design functionality.
For more information please contact:
Kim Brown
Vice President
(209) 940-5118
KBrown@deltafund.com
Experience the Delta Promise